Pancreatic cancer often eludes early detection because symptoms typically don’t surface until the disease is well established. This makes it important to respond appropriately to warning signs, even though some may be vague or caused by another health condition.
What are the symptoms of pancreatic cancer?
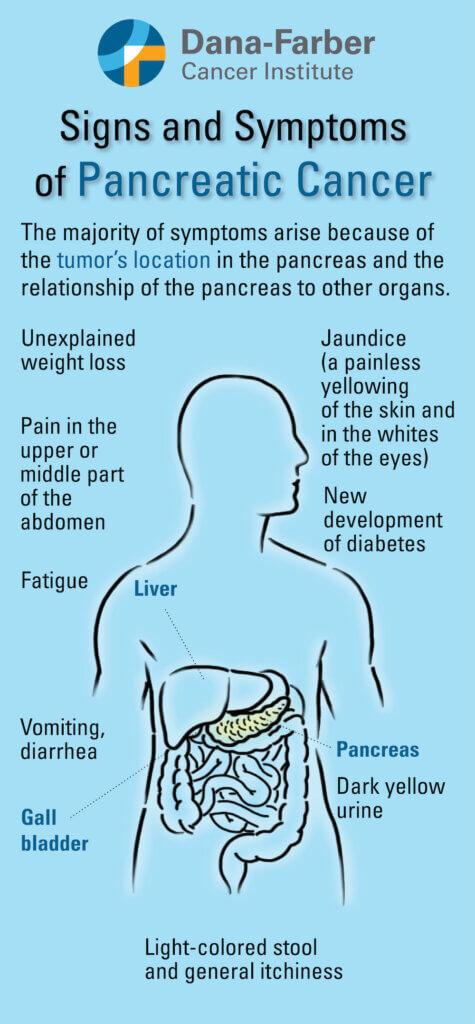
Most symptoms of pancreatic cancer are caused when tumors put pressure on organs and nerves, or close off pathways that move important hormones and enzymes through the body. Common symptoms can include:
- Jaundice: Jaundice, yellowing of the skin and eyes, is one of the most common symptoms of pancreatic cancer. This occurs when a tumor blocks the liver’s bile duct. Bile is needed to transport waste out of the body and break down fatty foods during digestion. Jaundice occurs because of a buildup of bilirubin, a yellowish pigment contained in bile.
- Dark yellow urine and/or light-colored stools: The buildup of bilirubin caused by jaundice can also cause your urine to turn a dark yellowish brown or cause your stools to become unusually pale.
- Itchy skin: Excessive levels of bilirubin can also cause itchy skin.
- Weight loss and/or lack of appetite: This can occur when a tumor presses on the stomach, making it difficult to eat and causing nausea. Pressure from a tumor can also close off the ducts that transport digestive juices to the small intestines, making it difficult for the body to absorb nutrients.
- Vomiting, diarrhea, and/or constipation: These symptoms can occur when the tumor presses on the intestines or changes the absorption of nutrients from food.
- Abdominal pain that radiates to your back: This can be caused by the tumor pressing on nerves or internal organs.
- Fatigue: The body’s fight against cancer can leave you tired even when you haven’t exerted yourself.
- New onset of diabetes: In rare instances, this can occur when cancer destroys the cells in the pancreas that make insulin and cause blood sugars to rise.
What does the pancreas do?
The pancreas is an organ about the size of your hand that sits between the liver, stomach, gallbladder, and bowel. Its primary function is to release enzymes that aid digestion and produce hormones, such as insulin, that manage blood sugar and digestion.
About 95 percent of pancreatic cancers begin in the organ’s ductal cells, which help move pancreatic juice to the small bowel. Other pancreatic cancers begin in the exocrine cells which produce enzymes that help the body eliminate waste or endocrine cells that make hormones.
How is pancreatic cancer diagnosed?
The first step is to speak with your doctor. Generally, initial testing will begin with laboratories, a CT scan, MRI, endoscopy, and/or other procedures to search for signs of pancreatic cancer. If your doctor determines that further testing is needed or a cancer is identified, Dana-Farber can schedule appointments to provide a comprehensive diagnosis and plan.
What are the risk factors for pancreatic cancer?
Nearly 63,000 people in the United States are diagnosed with pancreatic cancer each year.
Risk factors include:
- Age: Most cases are among people 55 and older. The median age of diagnosis is 71 years.
- Smoking cigarettes
- Obesity
- Diabetes
- Race: African Americans are at higher risk than white, Hispanic, or Asian American people
- A personal history of pancreatic cysts
- A family history of pancreatic cancer
- Chronic inflammation of the pancreas (pancreatitis)
- People with a genetic predisposition to pancreatic cancer
Is pancreatic cancer hereditary?
Yes, it can be. There are a variety of genetic predispositions that can trigger pancreatic cancer. These include:
- BRCA2, BRCA1, or ATM gene mutations
- Lynch syndrome
- Familial atypical mole-malignant melanoma (FAMMM) syndrome
- Multiple family members with pancreatic cancer without a known inherited gene mutation
Dana-Farber provides genetic evaluations at its Center for Cancer Genetics and Prevention. Talk to your doctor about whether it makes sense for you to get tested.
How can I reduce my risk of pancreatic cancer?
- Stop smoking: Dana-Farber offers several strategies to help you stop smoking. You can get specific treatment recommendations by calling the Smokers’ Helpline at 1-800-QUIT-NOW.
- Eat a healthy diet: This includes fruits and vegetables, whole grains, lean protein such as poultry and fish, and health fats such as nuts, seeds, and olive oil. It is also good practice to limit your consumption of red meat, high-fat dairy, saturated fats, and sugar.
What is the treatment for pancreatic cancer?
Treatment varies based on the stage of the cancer and its location within the pancreas and or other organs. Common treatments can involve some combination of surgery, chemotherapy, and radiation.
There are several other forms of treatment that are used when the cancer spreads to other organs. These include targeted therapies (using drugs that target specific mutations in the tumor), immunotherapy (using drugs to prompt the body’s own immune system fight the cancer), and stereotactic radiation (high-dose, focused radiation).
Dana-Farber takes great pride in treating you, not just your cancer. As our medical specialists work diligently to treat your cancer, we also provide a network of social workers, dieticians, pain experts, geneticists, and other support services to help you maintain your quality of life.
Get more detailed information on treatment.
About the Medical Reviewer

Dr. Wolpin received his medical degree from Harvard Medical School in 2001. He subsequently completed his residency in Internal Medicine at Brigham and Women's Hospital, and his fellowship in Medical Oncology at the Dana-Farber Cancer Institute. He joined the staff of DFCI and Brigham and Women's Hospital in 2007, where he is a medical oncologist and clinical investigator in the Center for Gastrointestinal Oncology. His research focuses on biomarkers and novel therapeutics in gastrointestinal malignancies, and mechanisms by which lifestyle factors interact with malignant risk and progression.

Good information! Thank you!