Key Takeaways:
- The “Whipple” operation (or pancreaticoduodenectomy) is the most common procedure performed when the tumor is confined to the head or neck of the pancreas.
- The procedure is complicated and lasts about six hours, and there are potential side effects — but it can be lifesaving treatment option for certain patients.
- The procedure should be managed by an experienced team.
What is the Whipple operation/procedure?
Many pancreatic cancer patients are diagnosed after the cancer has spread beyond the pancreas, making surgery a risky treatment option. But for those patients whose cancer is localized, surgery may be used to remove the tumor and prevent further spread. When the tumor is confined to the head or neck of the pancreas, the “Whipple” operation (or pancreaticoduodenectomy) is the most common procedure.
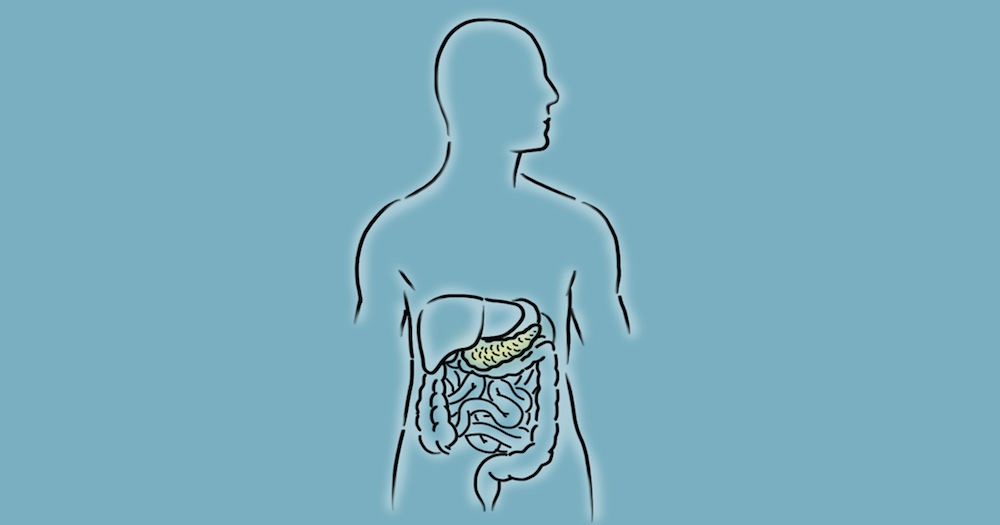
During the Whipple operation, a complex procedure lasting about six hours, surgeons will first check to make sure the tumor has not spread. They then remove the head of the pancreas; the duodenum, part of the small intestine; a portion of the bile duct; the gallbladder; and sometimes part of the stomach and nearby lymph nodes. After removing these internal organs, surgeons connect the remaining pancreas, bile duct, and small intestine so the body can digest food normally.
Following the procedure, patients usually spend five to seven days recovering in the hospital. They receive intravenous fluids on the first day after surgery and advance from liquids to solids over two or three days. They’re out of bed and walking the first day after surgery.
The Whipple procedure should be managed by an experienced care team. Quality is associated with experience: Studies show that higher surgical volume correlates with better patient outcomes. Experts in the Pancreas and Biliary Tumor Center at Dana-Farber/Brigham and Women’s Cancer Center perform hundreds of pancreatic and biliary cancer surgeries per year, including the Whipple procedure and new complex surgeries to remove tumors in patients who had not previously been candidates for surgery.
What are the side effects of the Whipple operation/procedure?
The Whipple operation requires an experienced team to anticipate and manage the many potential side effects, which may include:
- temporary leak of pancreatic fluid from the pancreatic connection
- infections
- bleeding
- slow emptying from the stomach after eating
- weight loss
- change in bowel habits
- diabetes
What are the long-term side effects?
Not all patients experience these long-term side effects, but they can include:
- decreased pancreatic function, in which the organ doesn’t produce enough enzyme to digest food in the small intestine. This can result in abdominal pain and tenderness, loss of appetite, and weight loss and diarrhea
- diabetes
- difficulty digesting fatty and/or sugary foods
Patients who undergo the procedure will also be closely monitored for signs that the cancer has returned.
What food should I eat after the Whipple procedure?
Dana-Farber nutritionists will often recommend patients eat small, frequent meals after the procedure until the stomach is able to empty itself properly. Patients also require close follow up to monitor for any evidence of diabetes or decreased pancreatic function.
Will I need more treatment after the Whipple procedure?
After surgery, further treatment, called adjuvant therapy, which may involve chemotherapy, is often recommended.
Compassionate care and support
At Dana-Farber, we consider each patient’s quality of life to be our top priority as we aggressively treat their cancer. Our medical, nursing, and support staff have a passion for caring for patients with pancreatic and biliary cancer, and we help each person through a medically and emotionally challenging time. We take the time to form one-on-one relationships with our patients and get to know them and their loved ones.
We offer support programs and resources that help patients and families, including nutrition counseling, complementary therapies such as massage and acupuncture, and support groups led by our social workers.
Learn more about treatment for pancreatic cancer, which may also require chemotherapy and radiation therapy, from the Pancreas and Biliary Tumor Center at Dana-Farber/Brigham and Women’s Cancer Center.
