When Liz Bowen first learned she would need a stem cell transplant, she had no idea she’d be making history as the first outpatient stem cell transplant patient in New England.
Bowen, 55, was diagnosed with cutaneous T-cell lymphoma, a rare form of skin lymphoma, in 2017. Her care team at Dana-Farber/Brigham and Women’s Cancer Center (DF/BWCC) immediately enrolled her in treatment, including radiation therapy and participation in a pair of clinical trials. The therapies relieved some of Bowen’s pain and itching, but did not put her into remission.
The next year, the U.S. Food and Drug Administration approved the drug mogamulizumab-kpkc, a monoclonal antibody, for rare types of lymphoma — including Bowen’s. After only a month on the drug, the results came back: her cancer was in remission.
“After all I had been through, it was such a relief to hear I was in remission,” recalls Bowen. “And for the first time in a long time, I was feeling really good.”
Next steps
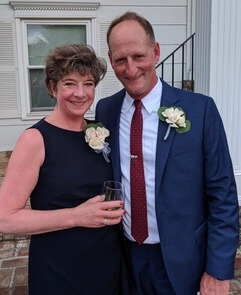
It was good news for Bowen, but her care team knew they couldn’t stop there: to further ensure that Bowen stayed in remission, they would need to add a stem cell transplant to her treatment plan. A stem cell transplant would replace the damaged and destroyed cells in her bone marrow with healthy cells, regenerating the blood cells and rebuilding a “new” immune system to better recognize and attack the lymphoma.
For the transplant, Bowen met with Corey Cutler, MD, MPH, medical director of the Adult Stem Cell Transplantation and director of the Ambulatory Transplant program at DF/BWCC, to discuss the logistics of an allogeneic transplant — a process in which a patient receives stem cells from a matching donor. In this case, they would be from Bowen’s sister.
While the stem cell transplant procedure isn’t new, what made Bowen’s case unique was that she had the option to enroll as the inaugural patient in DF/BWCC’s new ambulatory transplant program, the first of its kind in New England. The program is designed to reduce, or even eliminate, hospital stays for a portion of patients set to undergo reduced-intensity conditioning.
A less toxic treatment
A reduced-intensity allogeneic transplant, also known as a “mini”-transplant, is a modified form of the procedure that uses lower, less toxic doses of chemotherapy. Reduced-intensity transplants suppress the recipient’s immune system enough so the donor stem cells can take root — or “engraft” — there. The transplanted stem cells can then produce millions of healthy white blood cells, which mount an attack on the cancer cells that remain in the body. This is a phenomenon known as the graft-versus-leukemia effect.
“The goal of the outpatient transplant program is for patients to get their transplant without ever seeing the inside of a hospital,” notes Cutler. “This way, they can relax and recuperate in their home or local lodging with their caregivers.”
By participating in the program Bowen could forgo the typical process of being admitted to the hospital for four days of conditioning chemotherapy prior to transplant, and instead return home after each day of preparatory chemotherapy. She would also receive her new stem cells in the outpatient clinic and return for follow up appointments. Delighted with the idea of being able to finish every night in her own bed, Bowen leapt at the opportunity.
However, before she could start the process, she had one personal milestone she needed to celebrate. In June, Bowen headed down to Charleston, South Carolina to attend the wedding of her eldest daughter.
A big success
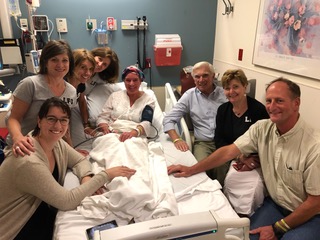
The following month, Bowen officially became DF/BWCC’s first ambulatory transplant patient. Looking back, she says she could not have been happier with her experience; the entire staff went out of their way to ensure she felt safe and comfortable.
“Being able to be in my own bed, surrounded by my things and the people I love, was amazing,” explains Bowen. “Everyone on my team took such good care of me, and I cannot say enough good things about all of them.”
“We are proud to be the first ones in New England to offer this program,” says Cutler. “Going forward, I believe this is something that patients not only want but may even seek out.”
Cutler’s team will now look to learn from and build off their recent success. As a result of Bowen’s outcome, they are scheduling more outpatient transplants with qualified patients.
With the transplant complete, Bowen has turned her attention to November 2020, when the family will head to New Hampshire to celebrate the wedding of their other daughter. In the meantime, doctors will continue to monitor Bowen for any side effects. She will regularly meet with her oncology care team and has a standing daily supportive care appointment that she can use if needed. This can be for anything from anti-nausea medication to administering additional fluids.
“We went into this with a big wedding, and we’ll be coming out of it with a big wedding,” laughs Bowen. “If you have the option to use this program, I’d encourage you to do so. I know it gave me a much better quality of life leading up to the transplant.”

Liz is such an inspiration for anyone facing a major challenge. I’m sure her experience will give many others the courage needed to pursue whatever course of treatment is needed to regain a full and meaningful life.
Liz Strong!
Wonderful. Congratulations Liz and family.
Dr Cutler is incredible as are his team members. I was part of that team for many years and actually the first outpatient allogeneic stem cell transplant occurred at DFCI approximately four years ago under the direction of Dr Cutler. Delighted to see this opportunity continues to be available to patients.
What an amazing story! So glad that Liz is doing well! My sister was treated at Dana Farber for a transplant and they did an amazing job! Great work, everyone!!!
Dr. Cutler and his team were fantastic when I had my AML transplant June 2014. Progress all the time. Never give up!!!!!!!!!!!EVER!!!!!!!!!!!!!!!!!!!!!!NEVER!!!!!!!!!!!!
Great Story!
Having gone through the “routine” allogeneic SCT in 2010, I would like to know more details about the process. I needed 24/7 nursing care. What is the home nursing care like? Are physician visits in the home or at DFCI? How are urgent medications delivered intravenously and by whom? How involved is the family in this care? I have too many questions! I am so happy she is doing well.
Wonderful!
Any work being done with Mesenchymal stem cells for perianal fistula?
Thank you for reading. Due to the high volume of comments we receive, we are usually unable to respond to each person individually. If you have a specific medical question related to this blog post, we would recommend talking to your doctor or other care provider. We’ve also gathered answers to some of the more frequent questions below:
-For more information on a particular type of cancer or the latest updates we have available, please visit our website (https://www.dana-farber.org/) or search our blog by clicking the magnifying glass at the top of our homepage: https://blog.dana-farber.org/insight/
-For information on whether you would be eligible for a certain treatment, please visit our website for more information on how to make an appointment or get an online second opinion: https://www.dana-farber.org/appointments-and-second-opinions/
-For information on clinical trials available at Dana-Farber and elsewhere, please visit the Dana-Farber database: https://www.dana-farber.org/research/clinical-trials/find-a-clinical-trial/. For clinical trials outside of Dana-Farber: http://www.clinicaltrials.gov.
Wishing you all the best,
Dana-Farber Insight team
Transplanted in 1996. Being able to do it at home would have been amazing. Being stuck in one room for a month was so anxiety provoking.
Best wishes for a speedy recovery.