by Richard Saltus
Cells are like young children – they need a lot of guidance on how to behave. Your body’s cells are constantly getting that help – in the form of hormones, growth factors, and other chemicals telling them when to rest, grow, duplicate their DNA, divide, or even self-destruct.
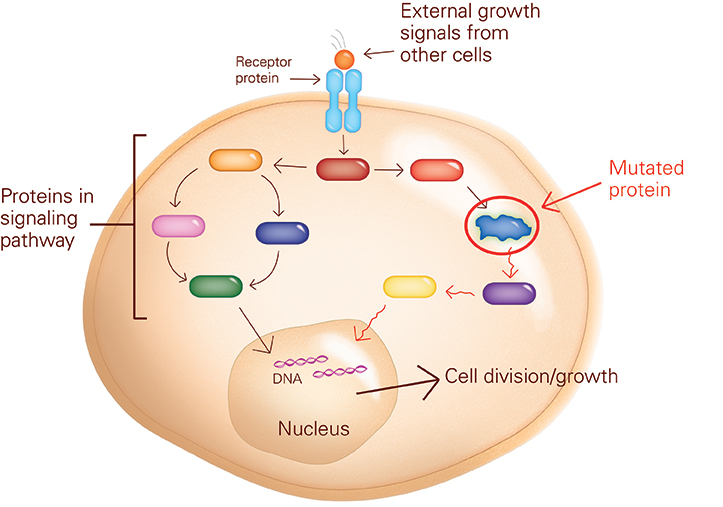
These commands are relayed from the cell’s surface to its nucleus by molecular pathways, also called signaling pathways, which are a series of interacting proteins that relay cellular messages, much as cell phone towers relay phone calls. When the commands reach the cell nucleus, they activate or turn off genes to determine how the cell responds.
Cancer often develops because of an error or mutation in a signaling pathway. For instance, an abnormal pathway may send growth signals to the cell’s nucleus even when no growth orders from the environment are being received at the cell’s surface. Here the altered pathway acts like a stuck “on” switch, so the cells divide uncontrollably, causing a tumor.
One of researchers’ biggest success stories has been identifying abnormal signaling pathways that have been hijacked by cancer cells to help them grow, spread, and become resistant to drugs. These discoveries have opened a new approach to cancer treatment that uses “targeted” drugs to disable one or more faulty proteins in the abnormal pathway. (The drugs are very selective because they are less likely to affect normal pathways in healthy cells.)
By blocking an overactive pathway, the drugs can slow a cancer’s growth and order malignant cells to self-destruct. Unfortunately, cancer cells can “learn” to activate other pathways, so that the original target drug is no longer effective by itself. Scientists then try to fight back by using combinations of drugs that attack multiple broken pathways.

Cancer is considered to be a dangerous disease. It is good to hear that cancer drugs can slow growth. Thanks for the information regarding this fatal disease and the way cancer cells progress.