Key Takeaways
- Bone marrow failure occurs when the bone marrow fails to produce enough healthy blood cells to keep up with the body’s needs.
- The most common cause of acquired bone marrow failure in children and adults is acquired aplastic anemia.
- Depending on the type, there are many ways to treat bone marrow failure.
Bone marrow failure occurs when the bone marrow — the soft, spongy center of the bones which is the site of blood formation — fails to produce enough healthy blood cells to keep up with the body’s needs. Bone marrow is the site where all blood cells are produced. These include red blood cells, which carry oxygen throughout the body via the protein hemoglobin, white blood cells, which fight infection, and platelets, which help blood to clot.
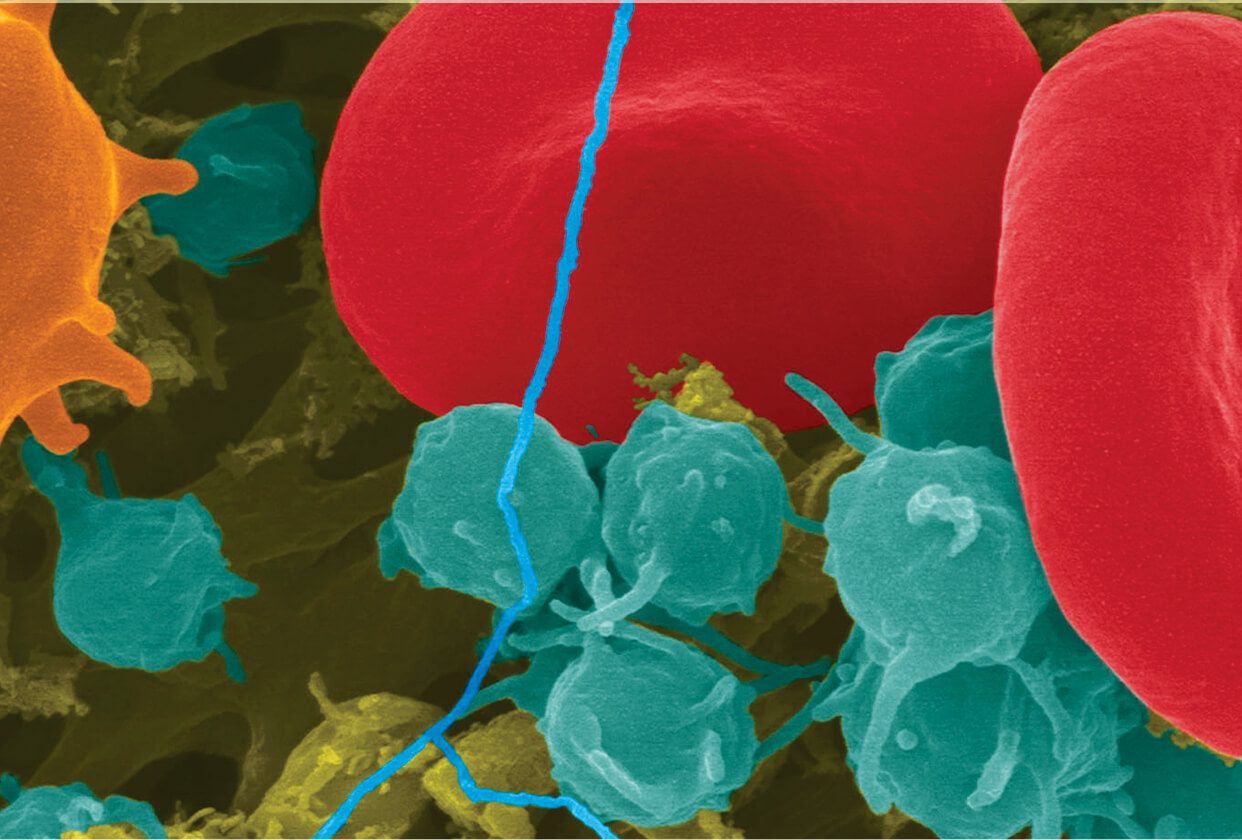
Depending on the types of blood cells that are comprised, bone marrow failure manifests in different ways. Many conditions may cause bone marrow failure, but in about 30 percent of cases, no specific cause is identified. Bone marrow failure can be inherited or acquired after birth.
What is the difference between bone marrow failure and bone marrow suppression?
Bone marrow failure should be distinguished from bone marrow suppression caused by an infection or drug, which improves over time. Bone marrow failure is most often not reversible.
What causes bone marrow failure?
The most common cause of acquired bone marrow failure in children and adults is acquired aplastic anemia. When the bone marrow’s hematopoietic stem cells are damaged, the body cannot make enough red, white, or platelet blood cells. Insufficient red blood cell production causes anemia, which has low energy as its main symptom. Decreased white blood cells raise the risk of infections. Low platelet production carries a risk of bleeding.
Acquired aplastic anemia differs from another disorder similar to bone marrow failure, called myelodysplastic syndromes (MDS), because even though the marrow fails to make enough blood cells, the few that are produced appear normal. With MDS, the bone marrow manufactures abnormal (dysplastic) cells that often have acquired chromosomal abnormalities. Both disorders are rare.
Some of the common inherited bone marrow failure syndromes are:
- Fanconi anemia
- Dyskeratosis congenital
- Diamond Blackfan anemia
- Shwachman Diamond syndrome
- GATA2-related disorders
- SAMD9/SAMD9L-related disorders
It is particularly important to think about inherited bone marrow failure in younger patients, as the major complications of these tend to develop with age. For example, it has been shown that Fanconi anemia can lead to aplastic anemia. Additionally, these disorders are associated with an increased risk of cancer, such as leukemia and solid tumor cancers.
How is bone marrow failure treated?
Depending on the type, there are many ways to treat bone marrow failure. Doctors sometimes provide supportive care, with treatments such as blood transfusions, to temporarily relieve symptoms. For example, a patient with thrombocytopenia, a condition characterized by abnormally low levels of platelets, can receive injections of platelets intravenously to control bleeding.
Bone marrow failure can also be treated with stem cell transplant. Otherwise known as a bone marrow transplant, a stem cell transplant involves is the infusion of healthy blood stem cells into the body to stimulate new bone marrow growth and restore production of healthy blood cells. This procedure takes advantage of the regenerative ability of the bone marrow. In one type of transplant, an allogeneic transplant, cells are collected from a tissue-matched donor, usually a brother or sister or an unrelated donor, whose human leukocyte antigens (HLA) are a compatible match.
Before receiving the transplant, patients undergo conditioning therapy, which includes chemotherapy and/or radiation, to prepare the body for the transplant. The goal of the conditioning therapy is to remove the diseased bone marrow cells to make space for the new healthy ones to grow. The conditioning therapy also suppresses the immune system so that the body doesn’t reject the donor’s foreign stem cells. The transplant stem cells are infused into the blood through an IV.
It takes about two to four weeks for the new blood cells to regenerate – during this period, the immune system is still weak and the patient is highly susceptible to viral, bacterial, and fungal infections. Bone marrow failure disorders are often complicated to transplant, so patients, both old and young, benefit from care at a center highly experienced treating these disorders.
Learn more about bone marrow failure from Dana-Farber Cancer Institute.
About the Medical Reviewer

Children with rare disorders, such as bone marrow failure and MDS, deserve the same level of medical care and the same chance to live a healthy life as children with more common disorders. We are striving to identify the causes of bone marrow failure and MDS to develop better treatments for these disorders. We partner with the patient, the family, and the referring physicians to work together as a team to develop and implement an individualized medical plan. My research spans basic scientific studies and clinical studies with the goal of improving the diagnosis and treatment of patients with bone marrow failure and MDS. Our patients benefit from access to the exciting scientific and clinical advances and cutting edge technologies developed by researchers at Harvard.
