Urinary problems are more common among older adults, when incontinence and urinary-tract infections become more prevalent and bladder cancer risk rises. About 9 out of 10 bladder cancer patients are above the age of 55, according to the American Cancer Society. The symptoms of bladder cancer can mirror those of other conditions, so it’s important to understand how bladder cancer affects the urinary system.
Bladder cancer is the fourth-most common cancer in men, who account for around 75 percent of cases. “We don’t yet know the reason for the male predominance of cases,” says Guru Sonpavde, MD, bladder cancer director at the Lank Center for Genitourinary Oncology at Dana-Farber Cancer Institute. “The increased prevalence in men does not appear to be related to smoking, chemical exposure and other risk environmental factors.”
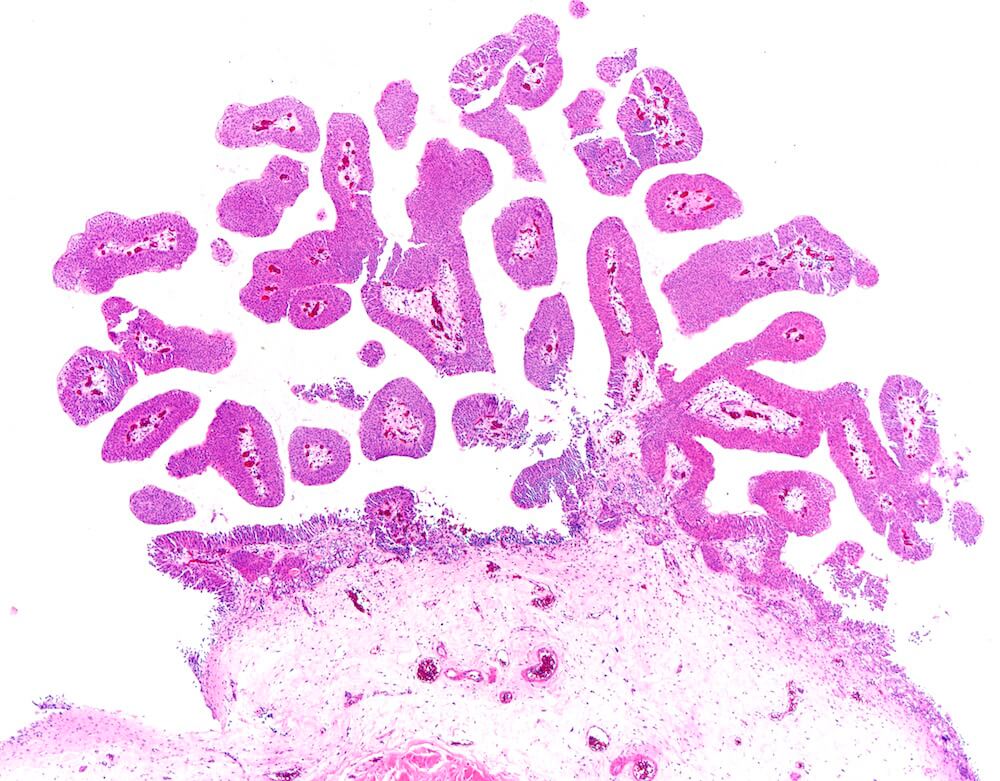
Bladder cancer first develops in the inner cellular lining of the bladder. Around 80 percent of cases are non-muscle invasive, meaning the cancer is only in the lining of the bladder, according to Sonpavde.
Bladder cancer tends to be caught at this early stage, when blood in the urine is a common symptom. “Tumors tend to be very vascular; there’s a lot of blood flowing through them,” Sonpavde explains. “Because of that, some tumors bleed and blood may enter the urine. Many times, this is mistaken for a urinary tract infection, especially in women. So it’s something to watch out for.”
Bladder cancer also causes patients to urinate more frequently. “The bladder might be irritated by the tumor mass and be unable to hold as much urine because of the tumor growing in it,” Sonpavde says. As a result, patients’ sleep patterns are often interrupted by their increasingly frequent nighttime bathroom visits.
As the tumor grows, it can cause pain and difficulty during urination. “More advanced tumors can cause obstructions in other areas of the urinary tract,” Sonpavde says. “The obstruction can cause trouble urinating and also lead to an infection.” An obstruction blocking the ureter connecting the kidney to the bladder can increase the risk of kidney failure.
When bladder cancer is detected at this early stage, the first-line treatment is a transurethral resection (TUR), which removes the cancerous cells and preserves the function of the bladder. This can be followed by an induction course of immunotherapy using the drug BCG, a weakened form of tuberculosis bacteria. BCG is injected into the bladder every week for six weeks, with the aim of triggering the immune system to attack the cancer cells.
However, if the cancer keeps recurring and/or progresses into the deeper muscle and fat layers of the bladder, then the patient might need a cystectomy. A partial cystectomy removes a portion of the bladder. Because the remaining bladder is smaller, patients will likely urinate even more frequently.
A radical cystectomy removes the entire bladder and surrounding lymph nodes. In patients with bladder cancer in the muscle tissue, chemotherapy is administered intravenously for two to three months before the bladder is removed. This step aims to kill cancer cells that have spread beyond the bladder and to improve the cure rate. Clinical trials studying immunotherapy might also benefit patients at this point as well.
In some cases, after the bladder is removed, a new bladder can be constructed out of a piece of the intestine. “However, bladder cancer usually occurs in older patients, who are less fit,” Sonpavde explains. “In those cases, they’re generally more likely to have a simpler procedure called an ileal conduit, which drains urine into a bag that comes out of an opening in the lower abdominal wall.” As they adapt to their newly rerouted urinary system, patients learn to incorporate the conduit into their daily self-care routine and work closely with their caregivers to monitor for any signs of recurrence in other organs or new tumors in urinary tract.

This is a very helpful summary. I was diagnosed early and am now undergoing BCG treatment