Stephan Bunker has learned to be prepared for anything during a half-century protecting others as a soldier, volunteer firefighter, law enforcement official, and director of 911 dispatchers for the state of Maine. So when Bunker was the one facing an emergency — a diagnosis of a brain cancer known as primary central nervous system (CNS) lymphoma — he was glad his doctor took the same approach.
Surgery and six months of chemotherapy had initially put Bunker’s cancer into remission, but his Maine-based oncologist knew there was a very strong likelihood it could come back. She offered to connect him with the Center for Neuro-Oncology at Dana-Farber Brigham Cancer Center, where Lakshmi Nayak, MD, was developing clinical trials to target CNS lymphoma.
Rather than take a “wait and see” approach against his cancer, Bunker seized the opportunity – one he hoped would help himself and potentially future patients through advanced understanding gained by the study.
“I’m not a guy to sit still,” says Bunker, 73. “If there are experts who are coming up with new ways to attack this cancer, and it can help me and others, I’m all for it.”
Bunker went to see Nayak, who found an immunotherapy trial for which he qualified. The results so far have been positive, and Bunker is back to saving others — and committed to spreading the word.
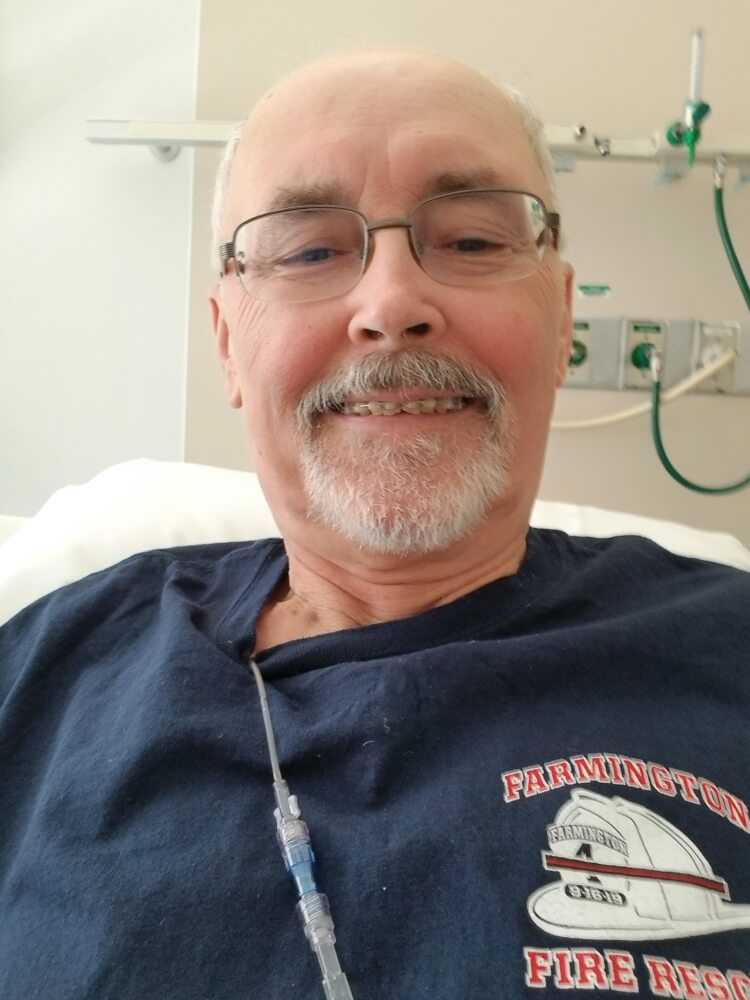
Trials and trepidations
Helping others has long been Bunker’s mantra. The son of a volunteer fire chief, he enlisted in the Army after high school and was a military policeman in Korea during the Vietnam War. He later earned degrees in law enforcement and criminal justice, and spent 25 years with the Maine Department of Public Safety as the first director of the state’s E-911 bureau. He’s also been a policeman, EM.T., teacher, selectman, and — for 43 years and counting — a volunteer fireman.
In March 2020, while enjoying “semi-retirement” with his wife Cheryl, Bunker developed “splitting headaches” that grew increasingly worse over 10 days. Pain medication did not help, but only when he began having mobility issues — another warning sign of CNS lymphoma — did Bunker feel concerned enough to visit his doctor.
“I was trained to be a tough guy, so I thought I’d gut it out,” says Bunker. “That almost cost me big-time.”
Initially, his primary care physician treated Bunker for a sinus infection. When the symptoms persisted, he sent him for a brain MRI.
“He got the results back that same day, on a Friday afternoon, and called me in immediately,” Bunker recalls. “Then he showed me the little spot behind my right ear and said he was scheduling me for neurosurgery first thing Monday morning.”
The March 31, 2020, surgery confirmed Bunker’s primary CNS lymphoma.
“My tumor was growing, and the doctors said it would have been inoperable if it got much bigger,” he says. “I was lucky.”
After a standard chemotherapy course of methotrexate at Maine Medical Center from April to September 2020 put the cancer into remission, he was referred to Nayak and Dana-Farber Brigham Cancer Center. Nayak suggested enrolling Bunker in an immunotherapy-based clinical trial. Immunotherapy harnesses the immune system, the body’s natural defense against foreign invaders, to attack cancerous tumors.
[Learn more about immunotherapy.]
“I didn’t know about immunotherapy or what it could do to my body, so I had some trepidations,” Bunker says. “Dr. Nayak was great at answering all my questions and put me at ease very quickly.”
The overall recurrence risk in patients with newly diagnosed primary CNS lymphoma after methotrexate-based chemotherapy is about 50% in the first two years. The risk is higher, however, for people older than 60 — like Bunker.
“We are focused on developing treatment options for consolidation that are safe, tolerable, and less toxic to the body as well as the brain, to reduce this recurrence risk,” says Nayak. “In this trial, after completion of induction chemotherapy, patients receive treatment with a checkpoint inhibitor, nivolumab, once a month for six months to determine if this immunotherapy approach will improve progression-free survival.”

Spreading the word
From November 2020 to April 2021, Bunker drove down from Maine once a month for immunotherapy, MRIs, and lab work at Dana-Farber Brigham Cancer Center. The only side-effect he ever experienced was an itching in his shoulders and upper arms, and he was able to maintain his firefighting and other activities.
These days Bunker has checkups each two months, alternating between Dana-Farber Brigham and Maine Medical Center, to make sure his cancer stays in remission. His Maine oncologist is in regular communication with Nayak to monitor Bunker’s progress. He says he feels “about 98 percent” like his old self.
True to his style, Bunker is now telling friends, fellow firefighters, and anyone else he can about warning signs for CNS lymphoma — and the importance of responding to them quickly and vigorously rather than “gut it out” like he initially did with his headaches. He is also dedicating himself to another cause: educating firefighters about the different cancers that they are more susceptible to from toxic chemicals encountered both on the job and on firefighting gear. Studies have found firefighters have a 9% higher risk of getting cancer and a 14% higher risk of dying from the disease than the general population.
“It used to be a badge of honor to have a dirty helmet or turnout gear, but now we know that this can be a sign of carcinogens we are being exposed to,” says Bunker. “Cancer has become the leading cause of death for firefighters across the country, and may well be what caused my brain cancer. We need to keep spreading the word.”

I am doing immunotherapy right now. The treatment got rid of my tumors. I still need treatments so they won’t come back. God is good.