Born on Jan. 1, Alan Morris is used to sharing a birthday with the New Year. Now the lymphoma patient also has a special day marking what he considers his rebirth — and a harbinger of hope.
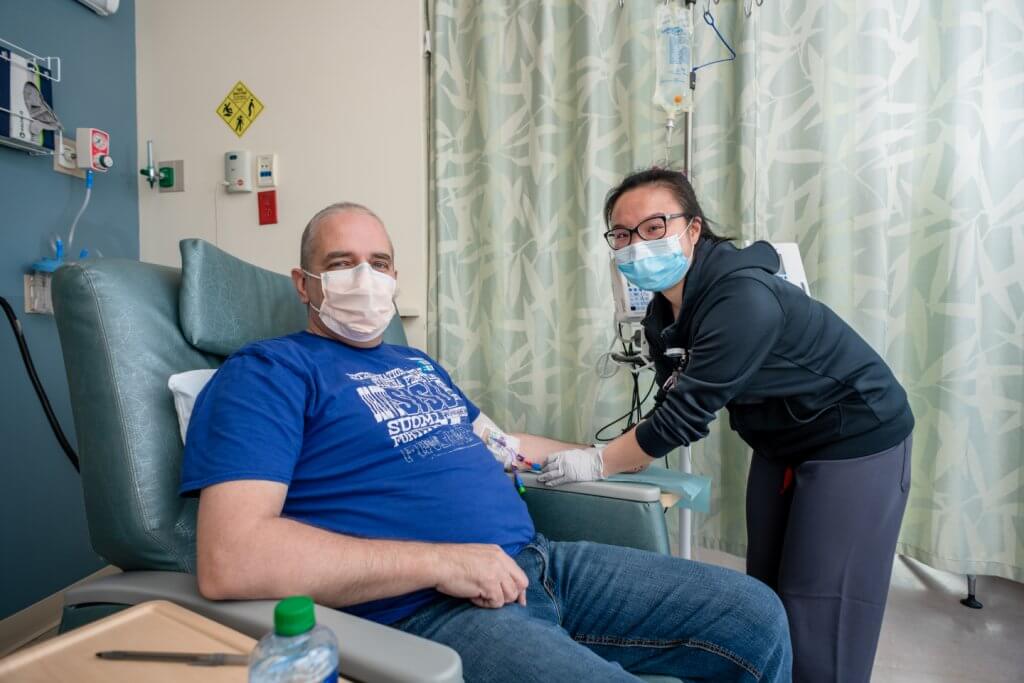
On Jan. 24, Morris, 58, became the first Dana-Farber Brigham Cancer Center patient to receive outpatient CAR T-cell therapy — a complex form of immunotherapy in which an individual’s T cells are collected, genetically altered to target a particular cancer, and then reinfused into the patient. The treatment generally requires a hospital stay of one or more weeks; the new outpatient option allows patients who live within a half-hour of Dana-Farber Brigham to return home each night while undergoing their prescribed daily monitoring in the outpatient clinic after receiving their CAR T cells.
“I feel excited — and lucky — to be the first [CAR-T cell therapy outpatient],” says Morris, whose infusion procedure came with wishes of “Happy Day 0 Birthday!” from his care team. “It’s great to be part of something new and promising.”
A good candidate
CAR T-cell therapy is the latest of many treatments Morris has undergone since his lymphoma diagnosis in October 2020. He tried several chemotherapy regimens, as well as radiation, at a hospital near his home in western Massachusetts. All failed to eliminate the cancer, and Morris was told he would likely need a stem cell transplant — which requires a lengthy hospital stay, major dietary restrictions, and months of isolation once the patient returns home. After his local doctors consulted with oncologist Austin Kim, MD, of the Adult Lymphoma Program at Dana-Farber Brigham, however, it was decided that Morris was a good candidate for the new outpatient approach.
“Because his lymphoma did not respond to two prior standard chemotherapy regimens, it was very unlikely that an autologous stem cell transplant would be successful in achieving a durable remission for Mr. Morris,” says Kim. “He is an ideal candidate for outpatient CAR-T cell therapy as he does not have a large volume of lymphoma or rapidly progressing lymphoma, and is less likely to have significant side effects.”
Morris and his wife, Becky, came to Dana-Farber Brigham in December for collection of his T cells — then returned for their reinfusion on Jan. 24. Because they live two hours away, they stayed at a nearby hotel for both procedures and the daily check-ups that followed. During this period, Becky played a vital role in her husband’s recovery.
“Our oncology nurse navigators educate all CAR T patients on what to expect, but outpatients and their caregivers receive extra education,” explains nurse practitioner Linda Ramsdell, MSN, FNP-BC, assistant program director of Immune Effector Cellular Therapy at Dana-Farber Brigham. “Becky will need to monitor Alan’s vital signs three times daily, use a special questions tool called an “ICE” score to assess his cognitive status, and record Alan’s progress in a workbook that our providers can review with them during their check-ups.”
Constant companions
Becky is also taught what side effects to look for — and who to contact if she spots them. As she and Alan work together to manage it all, hope and humor their constant companions.
“If I’m not sick of him after 16 year of marriage, this is sure to do it,” Becky jokes as she checks Alan’s latest handwriting sample. When she points out a misspelled word, he replies, “That doesn’t count — I couldn’t spell it right before!”
They miss their daughter, extended family, and beloved goldendoodle Thai waiting at home, but are grateful to be together.
“That means everything,” says Morris.
